What is Epidermolysis Bullosa?
Understanding EB & its classification
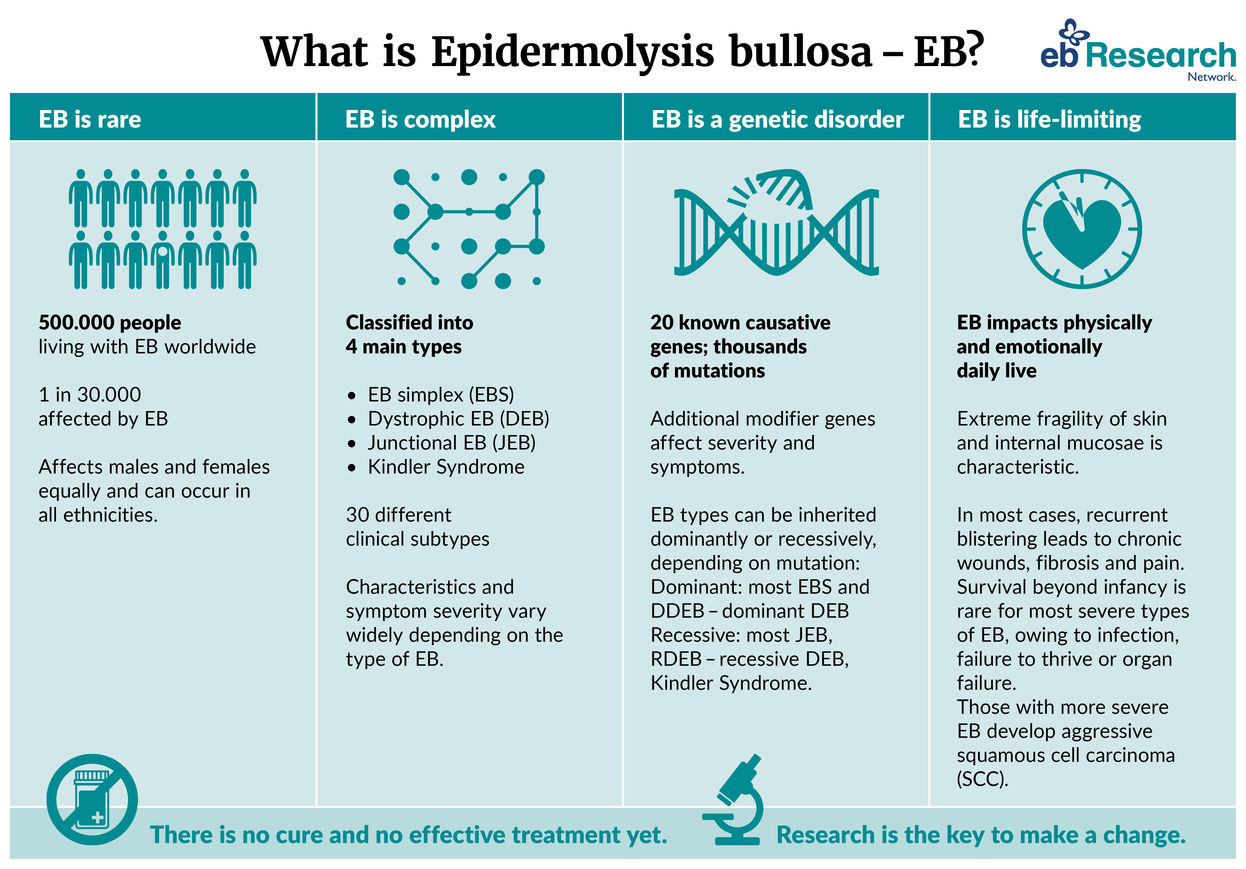
With a prevalence of only about 500,000 people worldwide, EB as a group of conditions is rare, and some subtypes are very rare.
EB is a group of inherited conditions where the skin and mucocutaneous membranes (i.e. membranes lining the mouth, gut, and corneal surfaces) blister readily with only mild trauma, friction, or apparently even spontaneously.
Classification of Epidermolysis Bullosa
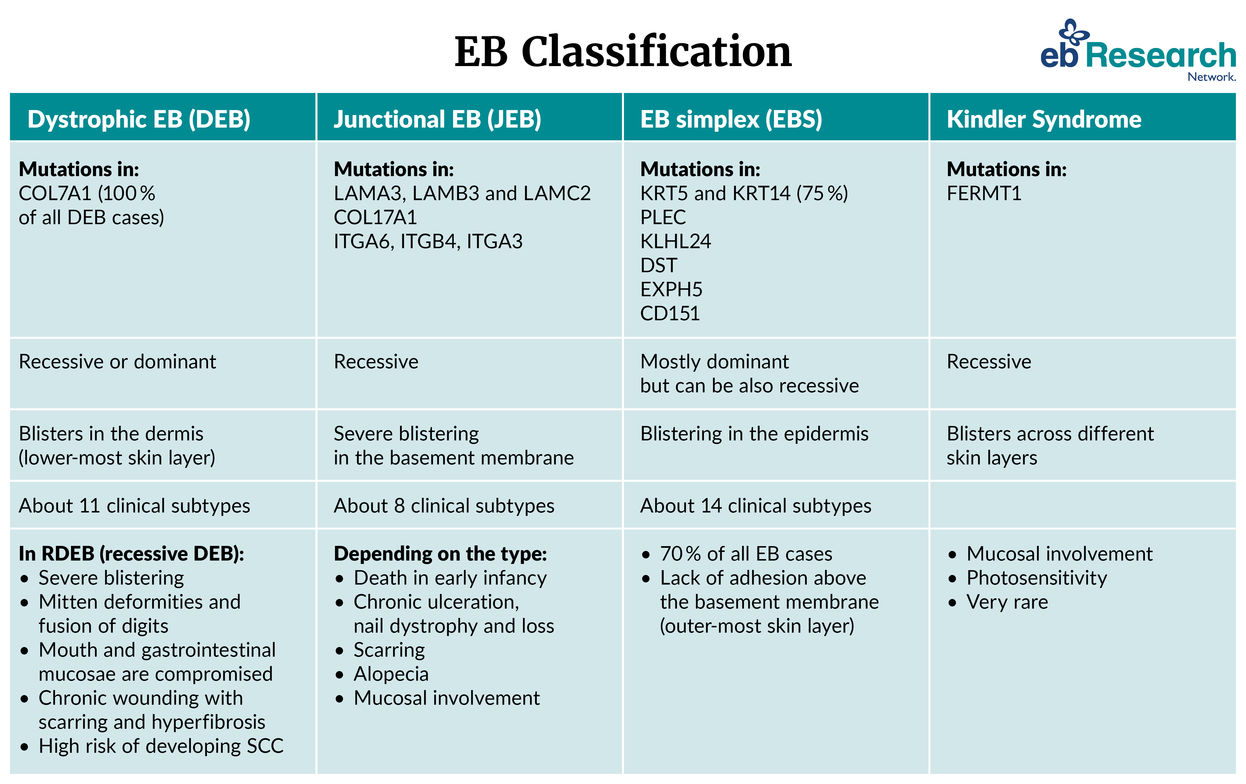
EB types are divided into four main groups according to the depth below the skin surface at which the blisters occur. Approximately 20% of EB cases are dystrophic (DEB), 10% junctional (JEB), and 70% simplex (EBS); Kindler syndrome is very rare. The genetic errors in EB result in defects in the proteins that make the outer skin layer (epidermis) adhere to the deeper layer (dermis). Some types of EB are inherited dominantly, others are inherited recessively. There are more than 30 clinical subtypes.
EB-Classification graphic below based on Has, C et al. “Consensus reclassification of inherited epidermolysis bullosa and other disorders with skin fragility.” The British journal of dermatology, 10.1111/bjd.18921. 4 Feb. 2020, doi:10.1111/bjd.18921
The first genes encoding proteins defective in EB were discovered in the early 1990s. There are now 20 genes identified in which mutations causing EB are known, with additional ‘modifier’ genes affecting symptom severity: all these constitute possible targets for therapy, symptom relief, and diagnostics. Nevertheless, there are many people with EB-like symptoms without mutations in known ‘EB genes’: identifying novel EB genes and mutations, and improving diagnostic technologies remain a priority for EB-ResNet.
Periodic review of the classification of EB types and EB-like blistering and other connective-tissue disorders, based on expanded clinical and molecular knowledge is undertaken periodically by EB-ResNet members and DEBRA groups. Downloads for the latest classification publications are provided below. A condition called ‘EB acquisita’, severe and symptomatically resembling RDEB, is not classified as EB, as it is an autoimmune condition against collagen VII, and cannot be treated using approaches appropriate to inherited EB.